Project members

Project
Many uropathogens are multi-drug resistant, adaptive immunity to UTI does not prevent recurrence, and BCG therapy does not always protect bladder cancer patients. These scenarios could be improved with established or experimental immunotherapy approaches, however, we need a better understanding of the bladder microenvironment in the context of disease.
The tumor immune microenvironment is an essential determinant of the response to immunomodulation in several cancer types. Identifying individuals who will not response to treatment would permit urologists to use alternative approaches to treat patients earlier, resulting in better outcome. In other malignancies, macrophages contribute to tumor eradication, or conversely, increased tumor growth or metastasis depending on the tumor microenvironment. We found that at least two macrophage subsets are resident in naïve (mouse) bladders and their divergent transcriptional programs translate to different functions in bladder infection.
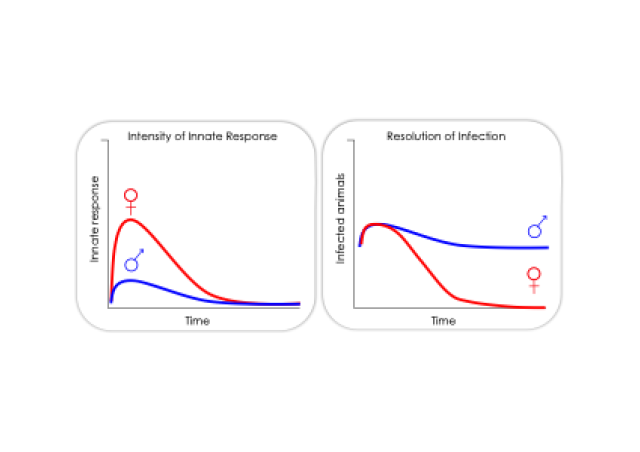
T cells are also crucial for long-term protection against tumor recurrence and their activity can be impaired by tumor-associated macrophages. In bladder tumors, complexity within T cell populations has not been well explored. We reported that while pan T cell infiltration is the same, tumor-specific T cells infiltrate male tumors better than female tumors in mice. Whether these macrophage and T cell subsets are found in bladder tumors and correlate with sex, age, or response to therapy is unclear.
Thus, to test whether macrophage and T cell populations predict response to immunotherapy for bladder cancer, we are identifying resident and infiltrating macrophage and T cell subsets and correlating these measurements with clinical characteristics to establish relationships among these populations and established risk factors for bladder cancer such as sex and age, as well as response to therapy in patients.